The concept of plantarisation describes a result of deformities. By clawing, twisting or overstretching joints, parts of the toes become a plantar contact surface that are not designed for this purpose. Ulcers are thus also created without high pressures. These changes concern parts of the foot that physiologically form the outline of the forefoot and the plantar side of the hallux at the IP joint. One third of all ulcers at DFS occur there. In the case of functional deformities that only occur under stress, this cause can remain undetected. It is then falsely suspected that the shoes have pressed the toes from the side or the front. An active search for plantarisation is therefore necessary. That is:
‘Every patient with ulcers in the toe area of the forefoot circumference and under the hallux may have a plantarisation. It is often not found without targeted examination.’
‘The cause of ulcers at the forefoot circumference and under the hallux cannot be attributed to tight or short shoes before plantarisation is ruled out.’
If the plantarisation can be observed at rest, the deformity is ‘static’. If it cannot be observed at rest, specific tests must be carried out for lesions on the tip of the toes, the lateral part of the fifth toe or the first toe. If it becomes obvious only then, the deformity is ‘functional’. If there is plantarisation at rest, it is examined whether the deformity can be corrected manually. If a correction is possible, the deformity is ‘flexible’, if not it is ‘fixed’. The fixation can be triggered by shrinkage of the joint capsule, ossification of the joint (ankylosis) or shrinkage of the tendons with effect on the joint. In fixed plantarisation, clinical and sometimes radiological examination can help to determine which structures contribute to deformity. Surgical procedures on tendons and capsules (soft tissue surgery) are generally less time-consuming, less complex and risky than operations on the bone. Soft tissue surgery, which is useful in the correction of plantarisation, includes the cutting of tendons, the lengthening of tendons, the transposition of tendons and capsulotomies. The latter refers to a plantar or dorsal slitting of the capsule to enable movement again. In the case of fixed deformities, capsulotomies or interventions on the bones involved in the joint may be necessary in order to achieve correct alignment and limit plantarisation.
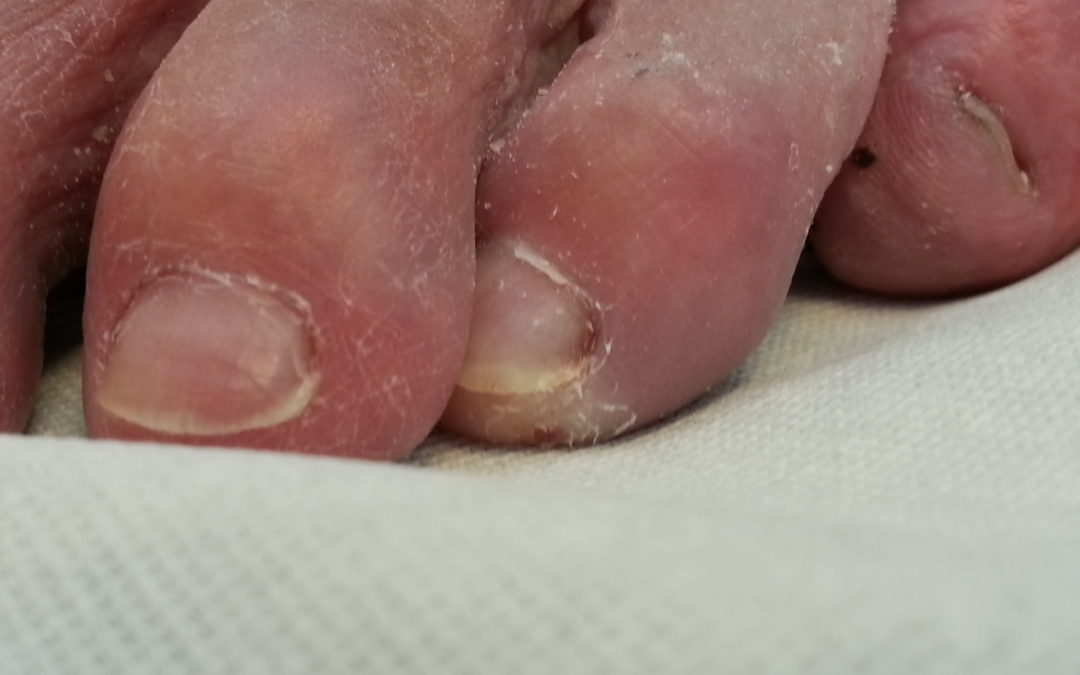
Plantarisation by hyperflexion (‘clawing’): In lesions at the tip of the toe, the unphysiological hyperflexion of the distal phalanx represents the plantarising deformity. The tips of the clawed toes become part of the weight-bearing surface in propulsion. The entire weight is carried by a very small area. To find this, the patient is asked to claw their toes. Then the examination is repeated while standing and the patient tries to stand on tiptoe. This is what happened when the cover picture has been taken.
Plantarisation due to torsion (‘twisting’): Torsion is a common phenomenon of the first and the fifth toe. At the hallux the medial side is twisted towards the ground, at the fifth toe, its lateral side is turned towards the ground.
Plantarisation by overstretching: At a hallux limitus, normal dorsiflexion in the MTP joint is increasingly restricted until complete stiffness prevents any movement (hallux rigidus). During propulsion, dorsal extension of the hallux is absolutely necessary. If this is not possible to be achieved in the MTP joint, this is compensated by overstretching in the IP joint. This joint usually does not allow dorsiflexion, but in this case a strong bend overstretches the joint and opens it on the plantar side. The sole areas of the joint, such as the condyles of the proximal phalanx, are not prepared for this strain.